Thank you for agreeing to be interviewed by me, Lucy Webster, Charity Co-ordinator of Diabetes Norfolk. We’re really interested to hear from you, particularly with regards to having a son with Type 1 and the journey you have faced and continue to face as a mum and a family to help raise awareness and help people not feel so alone.
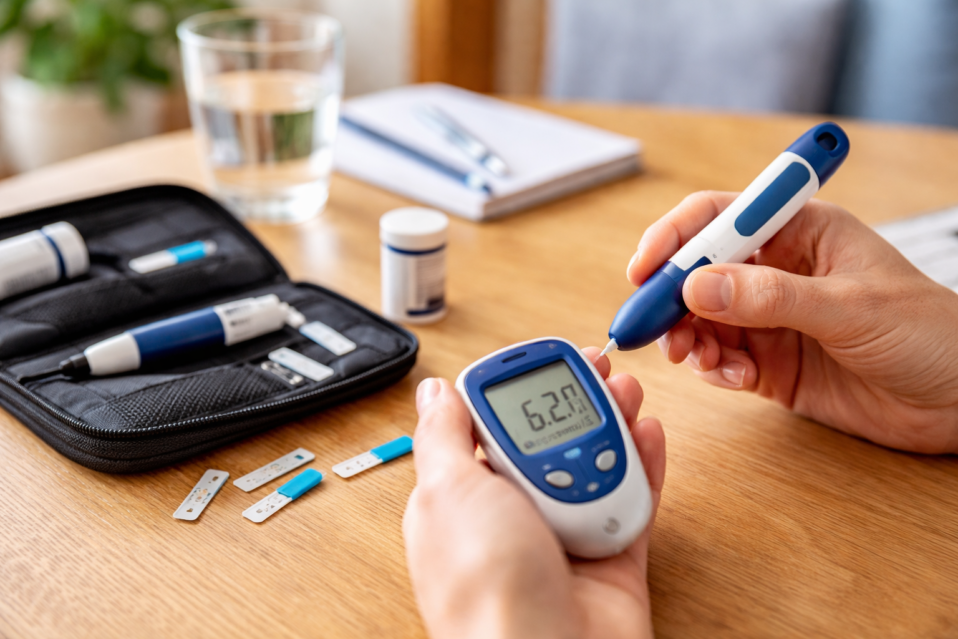
My journey was a very unexpected one as is anyone’s who faces a sudden, random type 1 diabetes diagnosis in their family to help raise aware. I wasn’t aware of type 1 diabetes. My son became unwell on holiday to Thailand – he become very thirsty and although he was eating many times a day was losing weight. On the flight home he became very ill with sickness and his eyes rolled back and he passed out which was absolutely terrifying. We took him straight to hospital where they asked: ‘do you know he has type 1?’ and I didn’t know what she was talking about but realised this is the horrible diabetes where you have to inject before food for the rest of his life.
I absolutely blamed myself and thought I must have done something wrong and it took me about 3 years to not blame myself. Prior to this diagnosis, about 7 months, my son was very poorly with daily sickness and our consultant said that type 1 can be virally induced so we think it was due to this.
I do whatever I can to raise money for the diabetes cause and to find a cure. It means so much to me that a cure is found. It has changed our lives so much as it becomes like an obsession and the thing that keeps my son going is technology. We were so pleased to move him from injections to the Omnipod. I was pushing for a pump but we had to do injections for the first six months and I wish there was more honesty that we would receive the pump in due course. This caused a lot of stress as we weren’t sure if my son would be able to access the pump and more advanced treatment.
If I could say one thing it’s to look after the parents too because the mental health stress is just ridiculous for parents as the children blame the parents and can cause resentment from having to continually remind the child to eat, inject, blood level monitoring, stress for managing the condition, the worry your child will have awful hypos in their sleep, etc etc. I would love for there to be a type 1 parent community set up where parents can go to. We wouldn’t have survived if we didn’t have a forum or Facebook community as NHS help is not there 24 hours a day so a dedicated website for type 1 where every question is answerable such as why does pasta affect my levels this way? Like a 24 hour hotline number with a library of information where people who have experience can help and support you – even in middle of the night when often horrendous hypos happen. I didn’t sleep for nights as I worried my son could die in the middle of the night from a hypo. Some enhanced support would be so much appreciated.
My son was lucky enough to have the Dexcom G6 where an alarm goes off to alert me of hypos. It totally changed my life. I joined the campaign to get the Dexcom available as well as looping. My son was so depressed and wondered why diabetes had happened to him and thought he must have done something bad for God to have given him this illness. I had to reassure him it was random. My husband and I decided to raise money and awareness to find a cure and helped my son with a belief system.
I raise money wherever I can and appear on TV shows where I can. I won £50,000 on Sitting on a Fortune and donated it to JDRF! I couldn’t believe my luck. I hope this will go to finding a cure. There is a race on now that there will be a cure and I look forward to this very much where there will be a day where I can turn to my son and say this isn’t going to happen anymore.
Is there enough support in your son’s education with managing diabetes?
It was difficult. On the plus side, the lunch ladies and school head were very helpful and sat with us and asked what they could do help – they weighed out his food. On the negative side, sometimes teachers would say, ‘sorry he’s got chocolate’ and I had to explain many times that he could eat it as he can adjust his insulin. I found this frustrating. This prompted me, as a form of therapy, to write a book called Bionic T1D. I want parents and children to have a book to feel more connected.
When my son was 6 I was invited to a charity event to hand out an award to children with diabetes. I met the young girl who received the award and the parents. Four years later my son gets diagnosed with type 1 and the same young girl was at the school! The mum helped me so much with diabetes support. You meet good people when you do good things. She introduced me to JDRF.
My OBE was due to 30 years of entertaining and charity work including Barnardos (my dad was an orphan in India), I have been a campaigner for kidney donations as I lost my mum to renal failure.
If you had three wishes to help diabetes in children what would they be?
1. A cure;
2. That the technology is so incredible that it is pain free;
3. That children aren’t treated any differently due to having diabetes.
Suggestions where a charity like Diabetes Norfolk could help?
100% Mental health support for both children and adults affected by diabetes. We had to pay privately as we were significantly affected as parents and so too was our son’s mental health. It took four years for the NHS to offer us any. Unless you have diabetes, or know someone personally, you don’t understand the level of stress you’re suddenly under. It is relentless! My son stopped eating as he didn’t want to inject or prick his finger and by stopping eating he thought he wouldn’t need to do this. He would rather starve himself than have the finger pricks! It’s the smaller things that matter. If money could be put towards a website and a hotline number to offer support it would be such a heavenly thing to have with a connection to mental health support too.
3 top tips for parents whose child has recently been diagnosed with diabetes?
1. Don’t underestimate the diabetes community on Facebook/internet with type 1 emphasis as is so very helpful.
2. Reach out to therapists as it is overwhelming and you need to let your feelings out.
3. Please join any charity that is helping to find a cure for diabetes.
I would say that when it comes to your child, to reassure them that a cure is coming and that this is the biggest day of their life as a cure is a real hope. Be there for them. There will be fights in the family so be prepared and it is okay – you will come out the other side. Hang in there!